Table of Contents
Definitions of obesity
Obesity can be defined as “a condition of abnormal or excessive fat accumulation in where health may be adversely affected”. The overall goal to classifying obesity is to identify individuals and groups that are at an increased risk of morbidity and mortality. Prevention and interventions can then be targeted to individuals or groups with greater accuracy, using predefined criteria.
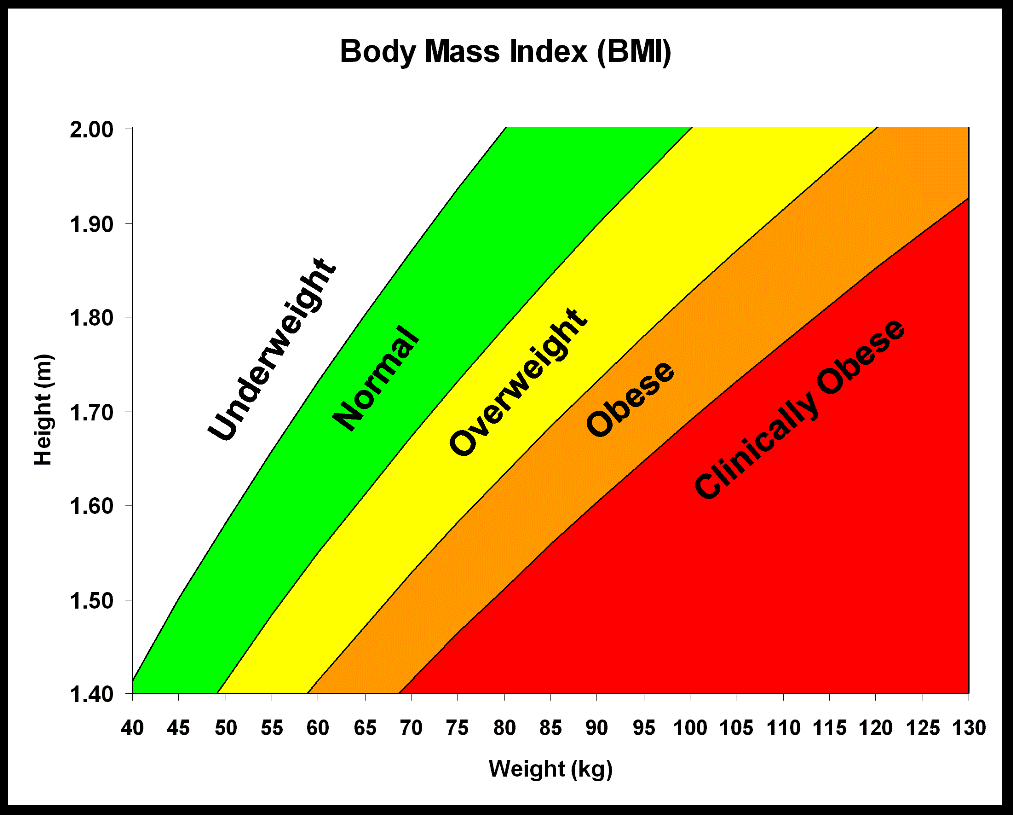
The World Health Organization (WHO) has chosen Body Mass Index (BMI) to quantify overweight and obesity. BMI is calculated as the weight (kg) divided by the square of the height (m). Overweight is defined as a BMI between 25- 29.9 kg/m2 and obesity is defined as a BMI ≥30 kg/m2. The association between BMI and impaired health is affected by, among others, ethnicity and age.
Lower BMI cut-offs has been proposed when assessing risk in subjects with Asian heritage, while higher cut-offs might be applicable in older people. There are pros and cons in adapting BMI cutoffs depending on age and ethnicity, and the WHO has thus far recommended the same definitions of overweight and obesity to be used globally, in all adults, and independent of age.
Central fat, located around the abdomen, is associated with a greater risk of disease than peripheral fat. To account for this, measures of central obesity have also been developed. The most commonly used measures are Waist Circumference (WC) and Waist to Hip Ratio (WHR). Indication of hazardous abdominal fatness is considered to be, WC>102 cm or WHR ≥0.90 for men; WC>88 cm or WHR≥0.85 for women.
More advanced measurement techniques allows for quantification of abdominal and gynoid fat masses. Abdominal fat is considered to be fat located on the abdomen, while gynoid fat is located at the lower limbs and/or around the hip area.
However, to date, there is no consensus on precise definitions of these fat masses, and there are therefore no specific recommendations on cut-off points.
Epidemiology of obesity
The prevalence of obesity is increasing worldwide and is considered to be the number one preventable cause of illness and premature death. By 2005, 1.1 billion adults and 10% of all children were overweight or obese and this figure is expected to continue to rise.
North and South America along with Western Europe have the highest proportions of obese individuals, while the prevalence is still relatively low in Asia and Africa.
In Sweden, there has been a steady increase in BMI over the past 30 years. The average BMI from 1980 to 2008 has risen by 1.66 kg/m2 in men and 0.76 kg/m2 in women. Also, the majority of men and more than one third of women are now considered overweight or obese.
In Sweden, about 14% are estimated to die due to effects of overweight and obesity. Due to the average increase in BMI, the present figure is 3% higher than just 30 years ago. (Estimates from figures provided by the Swedish central bureau of statistics and Banegas et al.).
Measurement of body fatness
Multiple methods for estimations of body fatness have been developed. The most common methods used in clinical and epidemiological settings include BMI, WC and WHR. For more precise measures of total body fat, dual energy x-ray absorptiometry (DXA) is often used.
Abdominal and visceral adipose tissue (VAT) is generally measured by computed tomography (CT), magnetic resonance imaging (MRI), or ultrasound.
Anthropometry
Anthropometric measurements provide approximate estimates of fatness and have the advantages of being quick, cheap, and readily available. BMI is most commonly used to estimate total body fatness and is correlated both to CVD risk factors and Cardiovascular Disease (CVD).
One of the downsides of the BMI scale is that it does not solely reflect fat, but it is also affected by muscle mass and skeletal weight.
To measure central obesity, WC, WHR, sub-scapular skinfold, and the ratio of sub-scapular to triceps skinfolds measurements are in practice.They are generally considered better than BMI at predicting CVD risk but they are poorly reproducible and still only provide crude estimates of abdominal or visceral fat.
Dual energy x-ray absorptiometry (DXA)
DXA is a low-dose radiation technique capable of measuring fat mass, fat-free mass (commonly referred to as lean mass), and bone mineral content. DXA is particularly good at assessing total body composition, but can also be used to estimate regional fat and muscle distribution.
New DXA technology is being developed that will be able to distinguish between VAT and subcutaneous adipose tissue (SAT), but currently there is no data available on the accuracy of this method.
The main drawbacks of DXA are the lower availability and considerably higher costs than anthropometric measures. The performance characteristics of DXA are covered in the Materials and Methods section.
Computed tomography (CT)
CT can accurately differentiate between SAT and VAT and is considered the gold standard for abdominal and visceral fat mass measurements. VAT is commonly calculated by a single slice image at the umbilical level, but volume can also be estimated from multiple slices.
Despite calculations being performed manually, CT has excellent inter- and intra-observer reproducibility.
Despite its good performance, CT is not commonly used in large-scale epidemiological studies due to the radiation exposure during examination, low availability and high costs.
Pathophysiology of obesity
Obesity is a complex disease, with no simple relationship between fat mass and impaired health. Simply focusing on fat mass is often inadequate. Some individuals have a high quantity of fat but low metabolic risk, while others with relatively little fat are at high risk of disease development.
This variation is largely dependent on two factors, size and location of adipocytes.
Adipocyte size and differentiation
During positive energy balance, increased storage of energy optimally occurs through the formation of added functional adipocytes through adipogenesis (hyperplasia). If adipogenesis is inadequate, or dysfunctional adipocytes are produced, this can lead to impaired uptake of glucose and free fatty acids (FFA), leading to ectopic lipid accumulation, decreased insulin sensitivity, and potentially type 2 diabetes.
The initial response of adipocytes during a positive energy balance is to increase in size (hypertrophy). This triggers paracrine signaling to produce more adipocytes with the purpose of maintaining adipocyte cell size and physiological functions.
Ultimately, whether the net effect to a positive energy balance is adipose tissue hyperplasia or hypertrophy is determined by genetic factors and actions of multiple regulatory proteins.
Examples of factors that promote hypertrophy are androgens (testosterone), inflammatory cytokines (IL-6 and TNF-α) and glucocorticoids, while catecholamines, estrogen and very low-density lipoprotein (VLDL) promote hyperplasia.
Fat storage
The pathogenesis of metabolic disease is influenced not only by the storage of fat (hypertrophy versus hyperplasia), but also by the location where the fat is stored. Adipose tissue can be divided into two major compartments: SAT and VAT. SAT is located underneath the skin, while VAT is located inside the peritoneal cavity surrounding the peritoneal organs.
The location is probably one of the main reasons why SAT and VAT have different pathogenic potentials. VAT secretes FFA and glycerol into the portal vein, thereby increasing hepatic triglyceride and glucose production, Obesity while promoting dyslipidemia and hyperglycemia.
Furthermore, VAT appears to be more metabolically active, with a high lipolytic activity that is less sensitive to the anti-lipolytic effect of insulin.
Other factors that are abundantly released from visceral adipocytes include pro-inflammatory cytokines (IL-6 and TNF-α), PAI-1 (decreasing blood clot degradation speed) and angiotensinogen (increasing blood pressure), which all contribute to increased CVD risk.
Subcutaneous tissue, on the other hand, is sometimes viewed as protective. During positive energy balance, small and well-functioning adipocytes can reduce circulating FFAs and thereby decrease the rate of atherogenesis. Even though SAT is not as harmful as VAT, it is still correlated to CVD risk factors such as diabetes, hypertension and hypertriglyceridemia.
Obesity and cardiovascular risk factors
The etiology of CVD is multifactorial and influenced by several factors in addition to obesity. Hypertension, dyslipidemia, impaired glucose tolerance, smoking, heredity, age and sex are some of the strongest risk factors of CVD and obesity is associated with several of these.
Most individuals that develop CVD have multiple CVD risk factors. The clustering of risk factors observed in many individuals is generally referred to as the “metabolic syndrome”.
There are several different definitions of the metabolic syndrome, but most are based on the presence of (abdominal) obesity, an unfavorable blood lipid profile, elevated blood pressure and insulin resistance.
Whether the use of these definitions improves clinical decision making compared to considering each risk factor individually is uncertain and has been a matter of debate.
Body Composition
Differences in body composition by age
There is great variability in the individual aging process. Changes in body characteristics are dependent on a large variety of factors besides chronological age, but the same trends in body composition are seen in most individuals.
For instance, a gain in body weight is commonly observed from age 20 to 60, and is primarily attributed to gains in adipose tissue mass. The gains in body weight are usually followed by a modest decrease after the age of 60, which is attributed largely to a decline in muscle mass.
After the age of 75, there is also a marked decrease in total body fat. In aging, there is a redistribution from peripheral to central fat and from subcutaneous to visceral fat. This age-associated decline in subcutaneous fat depots is accompanied by fat accumulation outside adipose tissue, e.g. in muscle, liver and bone marrow.
Changes in body composition are caused by a decrease in physical activity and by hormonal and nutritional changes.
Differences in body composition by sex
Sex differences in body composition are evident, beginning at the fetal stage and becoming more pronounced during puberty. Men have greater total lean mass and bone mineral mass, and less fat mass than women.
These differences are consistent throughout life and remain significant, even after adjusting for differences in height. Not only do men and women differ in body composition, but they also differ in their distribution of fat and muscles.

In women, the majority of fat is stored peripherally while men accumulate a greater part around the abdomen. Men have greater upper body muscle mass, while the difference in lower limb muscle mass is less pronounced.
Due to these differences, the WHO suggests using different thresholds for WHR and WC between men and women. BMI average, however, is similar in both sexes, so use of the same thresholds are acceptable.
Sex differences in body composition and fat distribution are largely due to actions of sex steroid hormones. In men, a reduction of free testosterone is associated with an increase in fat mass and reduction of muscle mass.
Correspondingly, estrogen deficiency in women is associated with an increase in visceral fat distribution. Even though women have a higher body fat percentage than men, they still have a lower risk of CVD.
One possible explanation for this is that men, on average, have more visceral fat than women. Also, hormonal differences are likely to play a role since estrogen has been proposed to reduce atherogenesis and hormone replacement therapy (HRT) has been suggested to reduce the risk of coronary heart disease in middle-aged postmenopausal women.
The protective effect of estrogen is attributed to actions on the vascular endothelial cells.
Activation of the estrogen receptor promotes production of endothelial nitric oxide, leading to smooth muscle cell relaxation and an inhibition of smooth muscle cell proliferation, ultimately resulting in a decrease in vascular tonus.
Even though there are positive theoretical effects of estrogen, it should be noted that HRT does not change or may even possibly increase the risk of CVD in the elderly.
Because of the increased risk for breast and endometrial cancer after HRT, this treatment is currently not recommended as primary prevention for CVD.
Positive effects of body fatness
In my view, the general public apprehension is that fat is harmful and should be restricted as part of our diet. Most people consider themselves to have a high fat percentage and would like to reduce their content of body fat.
Although this loss of fat would likely be beneficial, it is also important to recognize that not all fat is negative. On the contrary, fat is, in fact, crucial for our survival.
Throughout human history, weight gain and fat storage have been viewed as signs of health and prosperity. In times of frequent food shortage, holding a sufficient energy buffer has been essential for survival.
The overwhelming majority of calories are stored in the body in the form of fat. Even though muscle-derived proteins can be used as a long-term energy source, the subsequent loss of muscle mass is almost always disadvantageous.
The loss of muscle mass during starvation is less in individuals with larger fat reserves, and, in general, is less in females than in males. The higher ability for females to survive during times of famine are also well-documented.
Due to a limited food supply in much of human evolution, there has been a selection towards adiposity-promoting genes. The ability to store fat has not
only been vital to one’s own survival, but it is also important for reproduction and for passing on one’s genes.
Female fertility is particularly dependent on a certain amount of body fatness, as famine or anorexia nervosa are known to disrupt the menstrual cycle. Fat stores are also beneficial for pregnancy outcome, where low maternal weight and poor weight gain during pregnancy are known to result in low birth weight in infants.
Another important body function for survival is the immune system, which requires substantial energy to maintain optimal function. Negative energy balance reduces immune function and increases susceptibility to infections. On the other hand, by mechanisms not yet fully understood, immune functions also seem to be impaired in obese individuals.
Even with no apparent food deficit, underweight individuals have a decreased life expectancy compared to those of normal weight. Smoking and pre-existing disease likely contribute to the increased mortality associated with leanness, but a substantial part of the association remains unexplained.
Noticeably, most positive effects associated with fat are achieved by going from a state of underweight to normal weight, while health benefits going from normal weight to overweight are rare.
Negative effects of body fatness
As mentioned in the previous section, maintaining sufficient calorie intake has been a huge health issue during human evolution. Thus, individuals with a pronounced ability to accumulate fat had a competitive edge, so genes promoting fat accumulation were favored by evolution.
Now, as industrialization has lead to a significant decrease in the need for manual labor and food is abundant in large parts of the world, the pendulum has shifted so that obesity is becoming the main health concern.
Take, for example, the Pima Indians, who have excellent genetics for fat accumulation. In their traditional way of living, with a high degree of physical activity and low caloric diet, obesity was not a major health issue.
However, today, when most of these individuals live a modern western lifestyle, obesity and type II diabetes have reached epidemic proportions. In contrast, the Pima Indians who choose to live a more traditional lifestyle have significantly lower BMI, plasma cholesterol, and type II diabetes.
Modifying body composition and body fat distribution
In theory, losing total body fat is quite simple. By maintaining a negative energy balance, the body will eventually lose weight, most of which will probably be from fat depots. A negative energy balance can be established by either increasing total energy expenditure or by reducing calorie intake.
Body fat distribution is a bit more complex, since it is attributable to both genetic, endocrine, dietary, and lifestyle factors.
Exercise
Exercise increases calorie consumption, which would lead to a weight reduction. Often, though, an increase in physical exercise leads to a compensatory increase in food intake. Therefore, weight loss attempts with exercise, without dietary restriction, will only have a minor impact on total weight.
This does not, however, mean that exercise is ineffective in reducing obesity related disease risk. In fact, physical exercise will promote muscle build up and will reduce total fat mass if a constant weight is maintained.
With increased exercise, there is also a redistribution of fat, with a greater reduction in visceral fat mass. However, there appears to be no evidence that one can achieve site-specific fat loss by locally training a certain area.
Thus, fat reduction by exercise appears to be due to systemic rather than local effects, e.g. doing sit-ups is no better than walking, when trying to reduce abdominal fatness. Physical fitness is inversely associated with type II diabetes, CVD and mortality. These inverse associations appears to be independent of body weight.
Diet
As previously mentioned, restricting energy intake is vital to achieve and maintain weight reduction. Alterations in diet content, in addition to caloric restrictions, have been proposed to make it easier to maintain a negative energy balance.
Examples of weight-reducing diets are: low-fat, moderate fat (Mediterranean), high-protein, low-carbohydrate, and low-glycemic
index (GI). These diets have all shown positive short-term results, but maintaining weight after the initial weight loss has proven difficult on all of these diets.

The best diet for healthy obese individuals has been a matter of debate for a long time. The answer to this question will not likely be found in Body composition in the near future. Ultimately, it seems that the preferable diet is one that is long-term sustainable, and is a matter of personal preference.
Studying indirect mechanisms of diet can potentially provide new insights. Satiety is one of the factors that contributes to total energy intake. Proteins and fiber-rich foods provide a greater perception of fullness than fat- or simple carbohydrate-rich foods containing the same amount of energy.
Carbohydrate rich meals also, at least in the short term, suppress food intake more than high fat meals. Considering that fat is energy-dense and has a weak effect on satiety, decreasing the proportion of fat seems to be a theoretically logical way to reduce caloric intake.
Furthermore, as a high intake of saturated and trans-fats raises low-density lipoprotein (LDL) concentrations and increases CVD risk, these fats should undoubtedly be restricted to a minor part of our diet. It should, however, be emphasized that satiety is difficult to measure and that the number of studies in this field are limited.
Some people have argued that high-fat diets provide greater satiety than carbohydrate rich diets, but they seem to be only supported by indirect evidence of a larger initial weight loss on these diets.
For patient groups, there may be other factors, besides weight loss, to consider. For example, in a study of type II diabetes patients, a low carbohydrate/high-fat diet resulted in lower insulin, higher high-density lipoprotein (HDL) levels, and a greater reduction in visceral fat than with a isocaloric high-carbohydrate/low-fat diet.
Thus, for type II diabetes patients, a low carbohydrate diet might result in greater risk reduction than diets containing moderate- to high-carbohydrate content.
However, due to a lack of long-term studies, the Swedish Council on Health Technology Assessment has, thus far, concluded that there is insufficient evidence to specifically recommend low-carbohydrate/high-fat diets for diabetic patients.





